
Is saturated fat really that bad?





Coral Red: Mostly False
Orange: Misleading
Yellow: Mostly True
Green: True
Learn more about our fact-checking policies
Few dietary topics have generated more controversy, or more misleading headlines, than saturated fat. In one corner, decades of consistent evidence from health bodies worldwide linking it to raised LDL cholesterol and heart disease. In the other, a vocal online movement insisting it was never the problem at all, that scientists "cherry-picked" data, and that butter, red meat, and coconut oil are perfectly fine to eat freely. This guide walks through both sides, the science and the scepticism, clearly and honestly.
What is saturated fat?
Fat in food is made up of chains of fatty acids. "Saturated" simply means each carbon atom in the chain is bonded to as many hydrogen atoms as possible, there are no double bonds. This is why saturated fats are typically solid at room temperature: think butter, lard, the white fat around a cut of meat, or the solidified fat at the top of a cooled broth.
Unsaturated fats contain at least one double bond. They are liquid at room temperature, think olive oil, rapeseed oil, and the fat in oily fish. The practical difference between these two types of fat is significant, because they affect your cholesterol and cardiovascular health in notably different ways.

How saturated fat affects your body
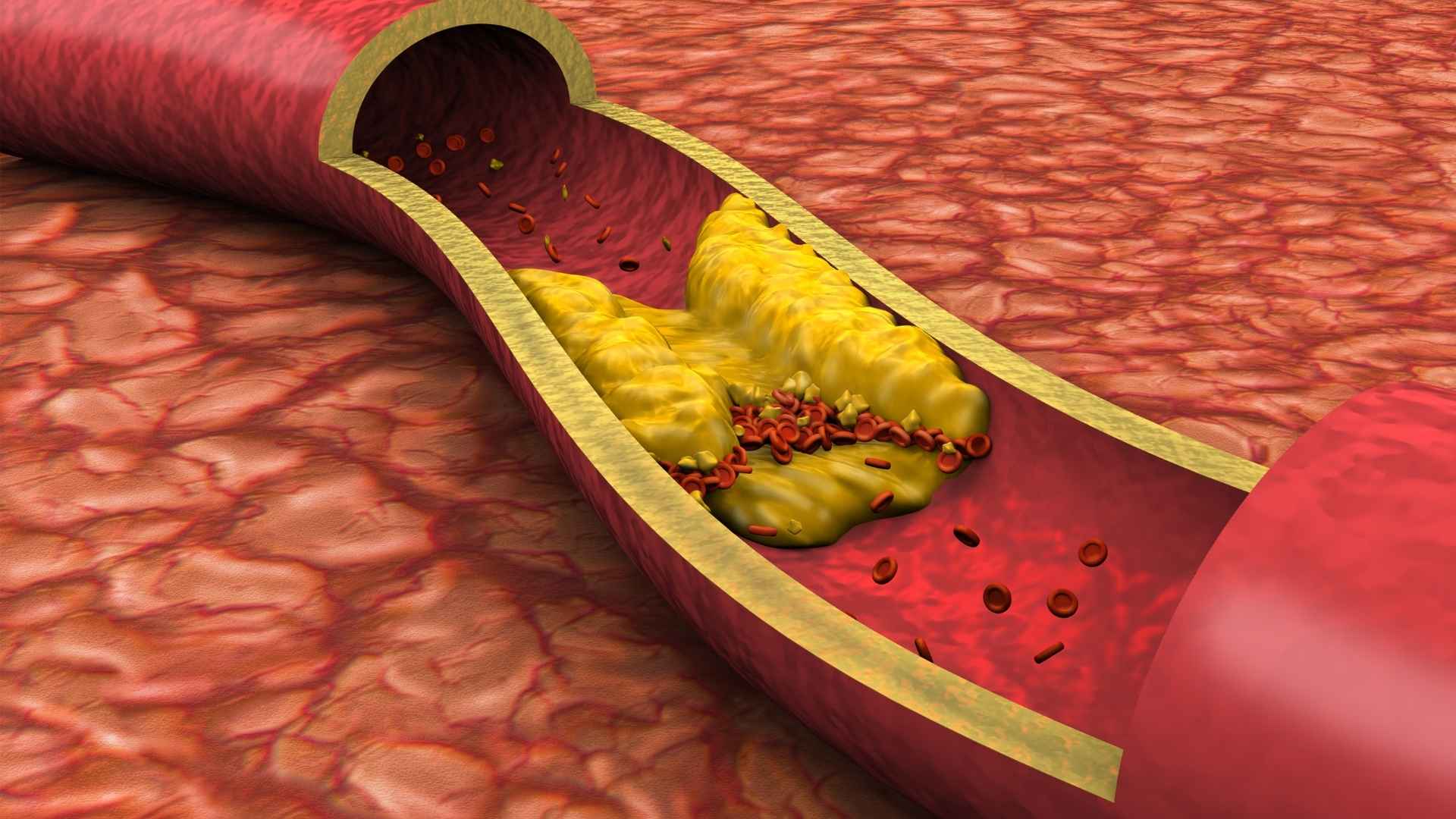
The primary concern with saturated fat is its effect on LDL cholesterol, the fatty particle that circulates in the blood and is strongly linked to plaque buildup in artery walls. Saturated fat impairs the body's ability to clear LDL from the bloodstream, causing blood levels to rise. High LDL is one of the most consistently supported causal risk factors for cardiovascular disease, not just associated with it, but shown through multiple lines of evidence to drive it.
The biological mechanism is well established: controlled feeding studies consistently show that increasing saturated fat intake, particularly the longer-chain saturated fats common in meat and dairy, raises LDL-cholesterol compared with unsaturated fats. Other lipid fractions can also shift, including HDL ("good" cholesterol) and triglycerides, but LDL remains the primary causal factor for heart disease and stroke.
A notable 2024 study, presented at the European Society of Cardiology Congress and funded by the British Heart Foundation, found that a high saturated fat diet caused around a 10% rise in blood cholesterol and a 20% increase in liver fat in just 24 days, with no change in body weight, isolating the fat itself as the driver.
What the evidence shows
Strong, consistent evidence from controlled trials, large population studies, and independent reviews shows that eating too much saturated fat raises LDL ("bad") cholesterol, a primary causal driver of heart disease and stroke. Major health bodies worldwide, including the WHO, the NHS, the UK's Scientific Advisory Committee on Nutrition, and the American Heart Association, recommend keeping saturated fat below 10% of daily calories and replacing it with unsaturated fats where possible. The claims that this advice has been "debunked" or "reversed" are not supported by the scientific evidence.
What the official guidance says
There is unusually strong alignment across global health institutions on this topic:
- WHO recommends saturated fat be kept below 10% of total daily energy intake, with further reduction towards 5% for additional cardiovascular benefit
- NHS advises men consume no more than 30g per day and women no more than 20g — the average UK adult currently exceeds these limits
- SACN — the UK's independent nutrition advisory body — reviewed 47 systematic reviews and meta-analyses in 2019 and concluded that the evidence to limit saturated fat intake and replace it with unsaturated fats remains robust
- American Heart Association recommends no more than 5–6% of daily calories from saturated fat for people with elevated cardiovascular risk
- HEART UK recommends an even lower ceiling — no more than 7% of energy — for people with high cholesterol
Despite this, UK adults consume around 12.3% of their energy from saturated fat — consistently above the recommended limit.
Where saturated fat comes from in the diet
According to HEART UK, 62% of the saturated fat in the UK diet comes from just three categories:
- Meat and meat products — including processed meats like sausages, bacon, and salami, which are among the highest contributors
- Cereal products — particularly biscuits, cakes, pastries, and savoury snacks
- Milk and dairy — especially butter, cream, full-fat cheese, and ice cream
Coconut oil deserves particular mention because it's frequently marketed as a superfood and "heart-healthy" alternative to butter. The reality: coconut oil is approximately 82–90% saturated fat, more than butter (63%) or beef fat (50%). As the European Food Information Council explains, claims that its medium-chain fatty acids make it uniquely healthy are misleading. While some of those chains don't raise LDL, they don't counteract the effect of the longer-chain fats in the same oil that do, and the net effect on LDL-cholesterol is similar to butter.

Why some people claim saturated fat isn't the problem
This is where the online debate gets most intense — and where the most misleading claims circulate. The sceptical case tends to draw on a handful of recurring arguments. Here's what they are, and where they fall short.
The Ancel Keys "cherry-picking" claim
The most popular version of this argument goes like this: in the 1950s, a scientist called Ancel Keys launched the Seven Countries Study, which linked saturated fat to heart disease. But Keys allegedly "cherry-picked" seven countries to support his hypothesis, ignoring 16 others that would have disproved it. Therefore, the entire dietary fat hypothesis is built on fraudulent foundations.
This story spreads widely in low-carb, carnivore diet, and food industry-adjacent circles — and it contains a kernel of truth buried under significant distortion.
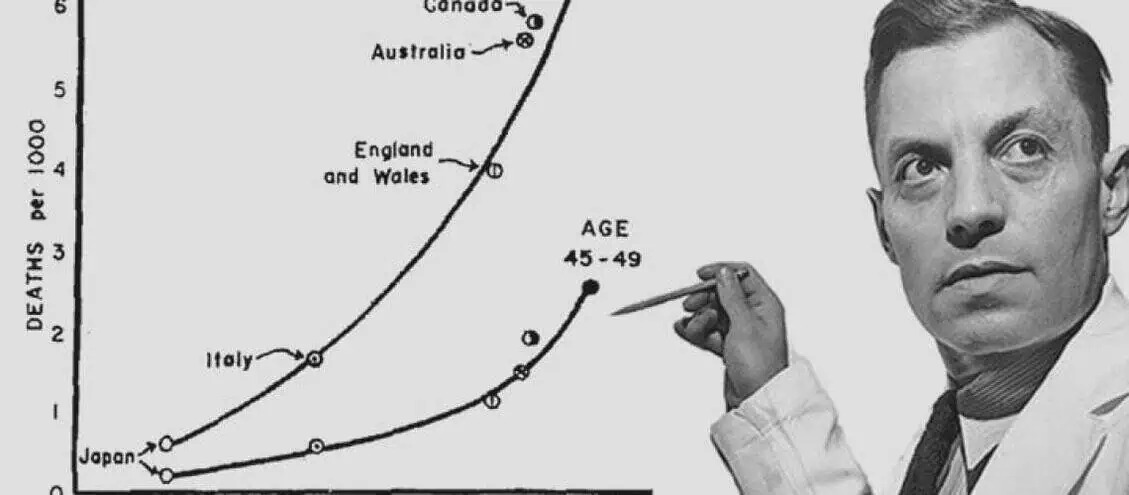
Yes, Keys used a non-random approach to country selection in the Seven Countries Study, which is a legitimate methodological criticism. But the claim that he "had data from 22 countries and ignored 16" misrepresents how the study was designed and how the data were collected, it wasn't a case of excluding inconvenient data points, but of choosing study sites prospectively. Furthermore, the "22 countries" graph that circulates online was created by a separate researcher from a different dataset, under different conditions.
More fundamentally, the diet-heart hypothesis doesn't rest on Ancel Keys alone. Decades of subsequent research, randomised controlled trials, prospective cohort studies, genetic studies, and controlled feeding experiments conducted across multiple countries by independent researchers, have repeatedly confirmed the relationship between saturated fat, LDL-cholesterol, and cardiovascular disease. Discrediting one scientist from the 1950s doesn't undo 70 years of converging evidence.
The "meta-analyses found no link" claim
Two studies are cited repeatedly by sceptics as proof that saturated fat has been exonerated: a 2010 meta-analysis by Siri-Tarino and colleagues, and a 2014 meta-analysis by Chowdhury and colleagues, both of which concluded there was no significant association between saturated fat intake and cardiovascular disease risk.
These studies generated significant media coverage, and they've been heavily misused ever since. The problem is that both have been subject to substantial methodological criticism.

The Siri-Tarino meta-analysis, on closer analysis, contained serious data errors, including reversed risk ratios — which when corrected shift the findings towards a positive association between saturated fat and coronary heart disease. When an updated meta-analysis was conducted including 21 studies published through 2014 and correcting for these errors, dietary saturated fat was associated with a statistically significant 15% increased risk of coronary heart disease.
A deeper flaw in both studies — and the one that most consistently misleads, is that they asked whether saturated fat is harmful compared to total diet, rather than asking the critical question: compared to what? When saturated fat is replaced with refined carbohydrates and sugar (which is what many people actually do), the cardiovascular benefit disappears. When it's replaced with unsaturated fats, the benefit is clear and consistent. The question was never "is saturated fat worse than nothing?" but "is it worse than unsaturated fat?" — and the answer to that remains yes.
The Nina Teicholz / "Big Fat Surprise" argument
Investigative journalist Nina Teicholz published The Big Fat Surprise in 2014, arguing that saturated fats have been unfairly demonised and that the evidence against them is far weaker than institutions acknowledge. The book was widely read and cited, and Teicholz has become a prominent voice in dietary guideline debates.
The core critique of Teicholz's work from nutrition scientists is that it applies selective scrutiny — highlighting methodological weaknesses in studies that support the diet-heart link while not applying the same critical lens to studies that undermine it. Her book focuses heavily on older observational data and largely dismisses the randomised controlled trial evidence, which provides stronger causal evidence and consistently shows benefits from replacing saturated fat with unsaturated fat.

Critically, it's worth knowing that Teicholz has publicly acknowledged that liberalising saturated fat is inherently linked to increasing meat and dairy consumption — and has described vegetarian advocacy groups as opposing her work for precisely that reason. That framing reveals how this debate is not purely scientific: it sits at the intersection of nutrition science, food industry interests, and dietary ideology. As foodfacts.org has previously explored, the the debate around the 2025–2030 US Dietary Guidelines followed this same fault line closely.
The "swap fat for carbs" false equivalence
One genuinely important insight from the low-carb community is that low-fat dietary advice in the latter half of the 20th century led many people to replace fat with refined carbohydrates, sugar, and ultra-processed foods — which caused its own set of health problems. This is a valid critique of how public health messaging was implemented.
But this does not mean saturated fat is fine. It means bad dietary swaps are bad. The evidence consistently shows that replacing saturated fat with whole food sources of unsaturated fat — nuts, seeds, oily fish, avocado, olive oil — improves cardiovascular health markers. The failure of poorly designed low-fat dietary advice is not evidence that high saturated fat diets are safe; it's evidence that dietary quality matters across the whole diet, not just one nutrient.

Where there is genuine nuance
Not all saturated fat behaves identically — and it's important to acknowledge where the science is more complex, rather than presenting a simple all-or-nothing picture.
The food matrix debate
Emerging research has explored whether the food matrix — the full physical and biochemical structure of a food — affects how its saturated fat is processed by the body. Full-fat dairy, in particular, has shown more neutral or even modest beneficial associations in some observational studies, which researchers attribute to effects like fermentation (in cheese and yogurt), the behaviour of fat globules in milk, and the presence of other bioactive compounds.
This is a genuinely interesting area of research, but it's important to keep it in context. The "dairy matrix" hypothesis is still emerging and largely based on observational data and in vitro studies. It doesn't overturn the broader evidence on saturated fat and cardiovascular risk, and it doesn't apply to butter, cream, or saturated fat from meat. It's also worth noting that research in this area is frequently cited by the dairy industry in ways that outstrip what the evidence actually supports.
Not all saturated fats are chemically identical
Saturated fatty acids vary in chain length — from short-chain fats (like butyrate in butter) to medium-chain fats (like those in coconut oil) to long-chain fats (like palmitic and stearic acid in meat and dairy). Some shorter-chain saturated fats appear to have less impact on LDL than longer-chain ones. However, most foods contain a mixture of chain lengths, which is why the net effect on LDL for foods like butter and coconut oil remains significant in practice.
This nuance does not support the conclusion that saturated fat is harmless overall — it supports the idea that the science is still refining its understanding of which types matter most.
What the best-evidenced diet looks like
The diet most consistently linked to lower cardiovascular disease risk across the broadest range of evidence is one rich in minimally processed plant foods — vegetables, fruits, legumes, whole grains, nuts, and seeds — with unsaturated fats (particularly olive oil and oily fish) as the main sources of dietary fat, and limited quantities of red meat, processed meat, and full-fat dairy.
This is broadly what the Mediterranean-style dietary pattern looks like in practice. It doesn't require eliminating saturated fat entirely — but it does mean reducing it significantly and replacing it with better options.
.jpeg)
Evidence also shows that plant-based meat alternatives — which are typically lower in saturated fat and higher in unsaturated fats and fibre than conventional meat — can improve LDL-cholesterol and support better heart health when used as a swap for red and processed meat.
Practical steps to reduce saturated fat
You don't need a complete diet overhaul. These are the changes with the most evidence behind them:
- Swap cooking fats — replace butter, lard, ghee, and coconut oil with olive oil or rapeseed oil for most cooking
- Reduce processed meat — sausages, bacon, salami, and other processed meats are among the highest dietary sources and also carry additional health risks beyond saturated fat
- Adjust dairy — semi-skimmed milk, lower-fat yogurt, and moderate amounts of strong-tasting cheese (so you naturally use less) all reduce intake without eliminating dairy altogether
- Eat more plants — beans, lentils, nuts, and seeds provide protein, fibre, and healthy fats without saturated fat
- Read food labels — the Food Standards Agency guidance is to aim for foods with less than 1.5g of saturated fat per 100g; more than 5g per 100g is considered high
- Watch hidden sources — biscuits, cakes, pastries, crisps, and many takeaways are significant contributors even when they don't taste "fatty"
Further reading on foodfacts.org
- Did the new US dietary guidelines clear saturated fat? — a detailed fact-check of specific claims circulating online
- The real war the new American dietary guidelines created — context on the political and scientific battle behind current guidance
- No, the medical community has not reversed its position on high cholesterol
- Are plant-based meat alternatives good for cholesterol?
- The firefighter analogy for cholesterol — fact-checked

Stand Against Nutrition Misinformation
Misinformation is a growing threat to our health and planet. At foodfacts.org, we're dedicated to exposing the truth behind misleading food narratives. But we can't do it without your support.
Sources
- American Heart Association (22 August 2024). Saturated fat.
- British Heart Foundation (September 2024). Research reveals hidden dangers of high saturated fat diet.
- Chowdhury R et al. (2014). Association of dietary, circulating, and supplement fatty acids with coronary risk. Annals of Internal Medicine.
- European Food Information Council (18 December 2025). Is coconut oil a healthy choice?
- Food Standards Agency (25 January 2018). Saturated fat.
- FoodFacts.org (22 October 2024). Fact-checking the firefighter analogy for cholesterol and heart disease.
- FoodFacts.org (18 December 2025). Are plant-based meat alternatives good for cholesterol?
- FoodFacts.org (30 April 2025). No, the medical community has not reversed its position on high cholesterol.
- FoodFacts.org (14 January 2026). The real war the new American dietary guidelines have created.
- FoodFacts.org (2 March 2026). Did the new dietary guidelines clear saturated fat?
- HEART UK (25 June 2024). Saturated fats.
- Kuijsten M (30 November 2024). Debunking the myths of Nina Teicholz's Big Fat Surprise.
- NHS (22 February 2022). Facts about fat.
- Public Health England (1 August 2019). Reducing saturated fat lowers blood cholesterol and risk of CVD.
- Scientific Advisory Committee on Nutrition (2019). Saturated fats and health. GOV.UK.
- Siri-Tarino PW et al. (2010). Meta-analysis of prospective cohort studies evaluating the association of saturated fat with cardiovascular disease. American Journal of Clinical Nutrition. PubMed
- Teicholz N (2014). The Big Fat Surprise. Simon & Schuster.
- Willett W (January 2026). Harvard T.H. Chan School of Public Health. Despite new dietary guidelines, experts encourage limiting red meat and full-fat dairy.
- World Health Organization (2023). Saturated fatty acid and trans-fatty acid intake for adults and children: WHO guideline.



foodfacts.org is an independent non-profit fact-checking platform dedicated to exposing misinformation in the food industry. We provide transparent, science-based insights on nutrition, health, and environmental impacts, empowering consumers to make informed choices for a healthier society and planet.

Was this article helpful?

















.svg)
